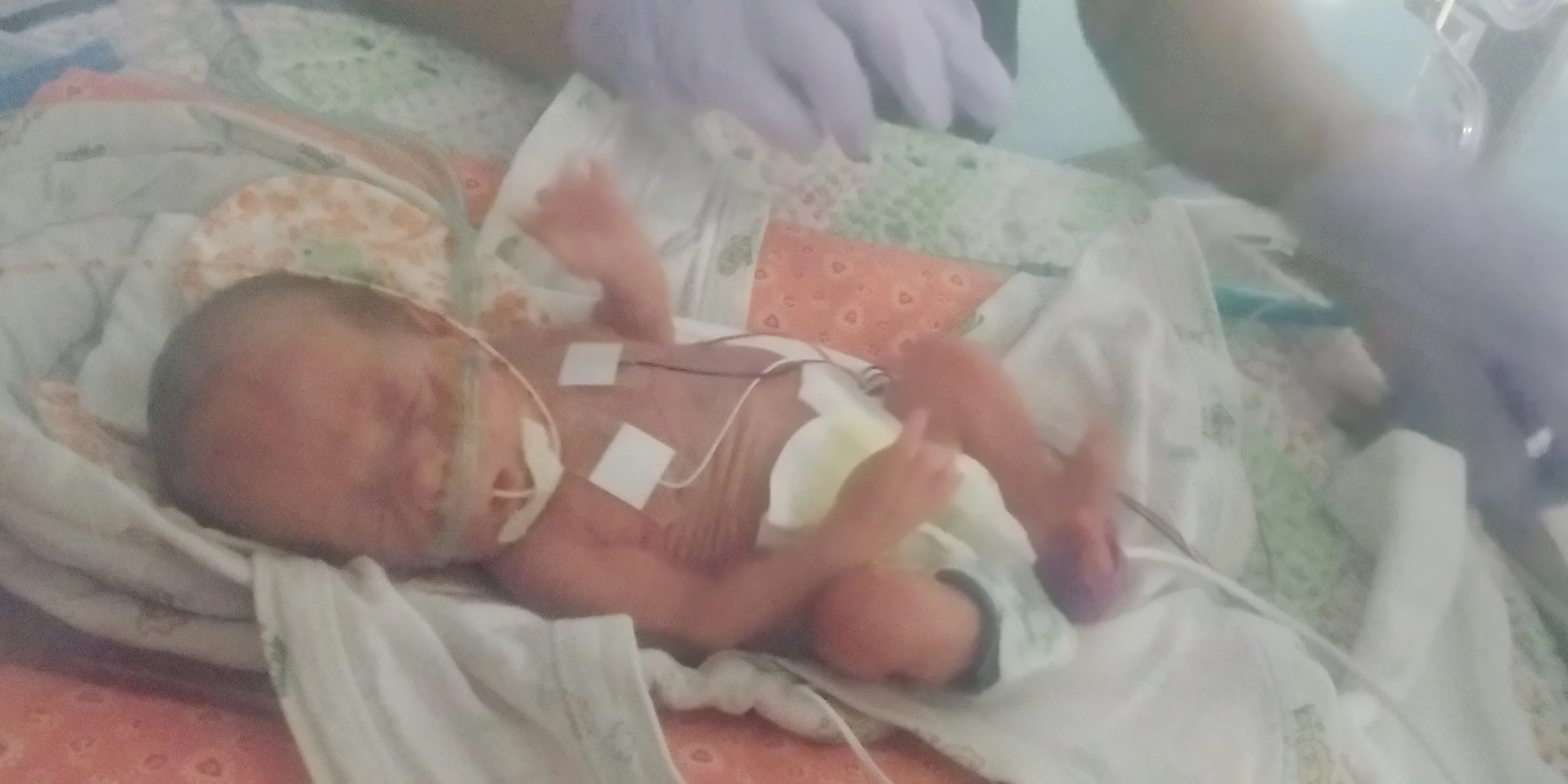
The babies qualify for lots of services. They also have lots of appointments. By way of example, since they have been home, Aubrey has had 4 eye exams, 4 appointments with a surgeon, 5 visits to the pediatrician, and has a visit to the pediatrician and a gastroenterologist this week; Finn has had 2 appointments with a pulmonologist, 4 visits to the pediatrician, and as a visit to the pediatrician and a gastroenterologist this week; Lydia has had 6 visits to the pediatrician, as a visit to the pediatrician and a gastroenterologist this week. They all will meet with a developmental specialist and Lydia has an appointment with a cardiologist and neurologist some time soon. They have been home for 6-7 weeks. That’s 24 appointments in 7 weeks. In addition to that, I have had to procure gauze, special wrapping for around Aubrey’s belly, mepilex, xeroform, and vitamins for the babies. I have had to get normal baby things (faster flow nipples (that’s a real thing), mylicon, more bottles, different bottles, etc.). We have also had to manage Lydia’s apnea monitor (it’s not too difficult, but if it’s not on right, it’s ear-piercingly loud), Finn’s oxygen and monitor (we had a power outage, we need to travel, it needs distilled water), and Aubrey’s twice daily care for his wound (which looks SO MUCH better!). I also have had to visit social security, am supposed to visit WIC (I tried once, but forgot some paperwork), and have had to talk to various agencies (CC4C, CDSA, maybe more…?). We have had visits from people who evaluate the babies, from people who bring medical supplies for the oxygen, and from people who pull data off of the monitors. It’s been really busy and without having such an amazing husband, I never could do it. We have also been very blessed to have help from our family with Lauren having been here for the longest period of time (and bringing up her boyfriend, Chris). She has helped keep some semblance of humanity in our home. Still, it’s been confusing. The long section below is primarily for me, but it might help someone know part of how these agencies work:
So, I had someone visit from CC4C (Care Coordination for Children) call me. I perhaps got a bit accusatory because when I had previously been contacted, they said they existed to help me schedule and coordinate care for the babies. I was so excited and told them how overwhelmed I was and that I could really use some logistical support. I don't know if I expected them to be my personal assistant, or what. But after explaining how much help I needed, the very nice lady said, "Great! Speak to you in a month!" and hung up. I was confused because how could she help me coordinate in monthly phone calls? So when I got a voicemail from them again, I called back and left a message saying that if they were just an extension of the nanny state trying to make sure I wasn't neglecting my children, I didn't need their "services" and I didn't have time for their foolishness. I was overwhelmed and overloaded and couldn't add another thing to my plate, particularly if they were there for people who had NICU babies as a result of some sort of drug addiction.
Well, I got a call back. Apparently, CC4C exists in NC to help children who were born to high risk homes BUT ALSO children who have special health care needs. CC4C is the one refers babies to a CDSA (Children's Developmental Services Agencies). The CDSA is the person who sends out a case coordinator (in our case, Sherri Crenshaw), who is the person who does the IFSP (Individual Family Service Plan). The IFSP sets what services the babies will receive.
The person from CC4C came out and reviewed the IFSP that Sherri had created for us and explained it. Apparently, Sherri felt that what I really truly wanted for my babies over the next 6 months was that they exclusively breast feed (WTF?!?!) and develop good suck, swallow, breath rhythms. I have no idea where she got that. I recall her asking what I had as goals for them and all I could envision was happy, well adjusted, healthy-haired, white-teethed, adults. So when she said "How does that they eat well sound?" I said, "Ok." Because, yeah. I want them to eat. But I also have NO idea what to expect of a 6 month old baby. Especially one who is straight outta NICU. I spent so much of my pregnancy worried about the babies making it to birth and then the entire time in the NICU worried about the babies making it out, I didn't spend any time researching or learning what developmental milestones I could/should expect. I know babies learn to sit up and roll over and babble and eventually do calculus, and I can put those in some sort of order, but not on a timeline.
The person from CC4C said that Sherri doesn't write the IFSP - I do. She suggested that I call Sherri back and explain what my actual goals are. We talked about my concerns (Lydia's reflux, Aubrey's giant hernia and how that will impact his development, and Finn's...well, I guess he's not a concern because he seems to be the most advanced, but then, that's on a barometer set by 2 other preemies). She said I need to tell Sherri that and tell her that I want more services. She did say that OP and PT might not be right right now, but play therapy certainly is. And she said that I can demand play therapy much more often. If I can handle it, 1 hour/week/baby. (Right now, Lydia and Aubrey get 1/2 hour every other week.) She also said that resources are limited so CDSA is encouraged, even if not explicitly, to offer minimal services. She said that parents really have to advocate for their children to fully get what they need from the programs.